Your IVF Journey Starts Here
At Tender Palm IVF, we are committed to helping you through the journey of parenthood. We understand the difficulties associated with infertility, and our sophisticated IVF treatments have helped thousands of couples to conceive.
There are preparations one needs to undertake before IVF. These include knowing the procedure, living healthy habits, controlling your emotions, and financial planning. The process entails fertilizing an egg with sperm in the lab, resulting in producing the embryo, which is then placed in the woman’s uterus for an increased possibility of getting pregnant.
Here at Tender Palm IVF, we are there for you at every step, from expert advice, compassionate care, and the highest quality treatment.
Keep hoping and be well-informed; now is the right time to get the first step toward your parenthood dream at Tender Palm IVF.

What is the process of IVF at Tender Palm?
Step 1: Evaluation and Personalized Strategy
Normally, a woman grows one egg per menstrual cycle, but IVF demands more than one egg. Several eggs enhance the chances of developing a viable embryo. To stimulate a woman’s ovaries, there is an injection of fertility hormones through which she may produce several eggs. To monitor the production of eggs, the doctor performs regular blood tests and ultrasounds, and your doctor will let you know when to retrieve the eggs.

Step 2: Ovarian Stimulation
The stimulation phase begins on Day 1 of your cycle. During IVF, medication will be administered for eight to fourteen days to encourage your ovaries to produce multiple eggs instead of the usual single egg.
Your specialist will provide personalized medication, typically in injection form, which can be given once or twice daily. While self-injecting can be daunting, your fertility nurse will guide you through the process, and it’s helpful to involve a partner or support person for extra reassurance. With practice, it will soon feel routine.
The injections often contain hormones like follicle-stimulating hormone (FSH) and luteinizing hormone (LH). Throughout the cycle, your specialist and nursing team will monitor your ovaries and follicle growth via blood tests and ultrasounds, adjusting your medication as needed.
As the stimulation phase concludes, monitoring will increase to time the ‘trigger injection,’ which prepares the eggs for ovulation. Your fertility nurse will inform you of the precise timing, as the egg retrieval must occur before ovulation.

Step 3: Egg Retrieval
The egg retrieval procedure, often called egg pickup (EPU), takes place at a hospital on the same day. During this procedure, a fertility specialist collects eggs from your ovaries. An anesthetist will provide general anesthesia, allowing you to be asleep during the procedure, which usually lasts around 20 to 30 minutes. Your specialist employs advanced ultrasound technology to accurately guide a needle into each ovary. This delicate procedure requires high precision, as even the smallest millimeter matters. Our specialists are exceptionally skilled in this area. Eggs cannot be seen with the naked eye; they are encased within fluid-filled follicles in your ovaries. Therefore, your specialist will extract the fluid from the follicles that appear to have developed sufficiently to contain an egg. Your fertility team has closely monitored your cycle, so they will have a good estimate of how many eggs they anticipate retrieving during the procedure. On average, between eight to fifteen eggs are collected, although this can vary based on your age and medical history. Following the procedure, you will awaken in the recovery area, where we will ensure you stay warm and comfortable. Approximately 30 minutes later, you will be able to walk out on your own. It is advisable to have someone accompany you, as you will be unable to drive after the EPU.

Step 4: Sperm Collection & Preparation
If you and your partner are considering the use of fresh sperm, one individual will need to provide a sample on the morning of the egg retrieval. For those opting for frozen or donor sperm, our lab team will have it prepared in advance. We evaluate the sperm based on four distinct quality levels. The laboratory is dedicated to preparing the samples to extract the most viable sperm for combining with your eggs, enabling our scientists to identify the best sperm using advanced microscopes. We take meticulous care in preparing the sperm before it is introduced to the eggs, employing various techniques tailored to each patient’s sample. The optimal sperm is one that is neither too fat nor too thin, with a tail that is of appropriate length, and is described as having normal morphology (shape/structure). Our scientists cultivate the ability to recognize morphologically normal sperm over many years, refining their skills continuously to select the most suitable sperm for each egg. Once the sample is adequately prepared, it is kept ready in the lab for the subsequent step. We then introduce the prepared sperm to the eggs collected during your egg retrieval procedure.

Step 5: Fertilization in the Lab
Your fertility specialist provides our scientists with eggs retrieved from your ovaries, stored in tubes with follicular fluid. Using advanced microscopes, our scientists locate and remove the eggs.
After retrieval, we culture the eggs in an ideal environment before insemination, either through standard methods or Intracytoplasmic sperm injection (ICSI), as determined by your specialist based on your situation to maximize fertilization and pregnancy success.
Following insemination, we place the eggs into specialized incubators and check for fertilization signs about 17 hours later. We look for two pronuclei, which indicate successful fertilization by one nucleus from the egg and one from the sperm. If two pronuclei are absent, the egg has not fertilized and will not develop into an embryo.

Step 6: Embryo Development
Ideally, fertilization occurs about 17 hours after the sperm meets the egg, leading to embryo formation. Our scientists cultivate the embryos in a specialized incubator, optimizing conditions for growth.
We create ideal growth conditions using a blend of amino acids and nutrients like those found in the body. Our goal is to mimic natural processes closely.
Over the next five to six days, we monitor the embryos, aiming for a two- to four-cell embryo by day two, a six- to eight-cell embryo by day three (cleavage stage), and a roughly 100-cell blastocyst by day five or six.
We aim to grow all embryos to the blastocyst stage, as this increases the chances of a successful pregnancy. Not all eggs will fertilize or develop properly due to maturity or sperm strength.
We will keep you informed about the development of your eggs, sperm, and embryos. If you have questions, our friendly team is just a phone call away.
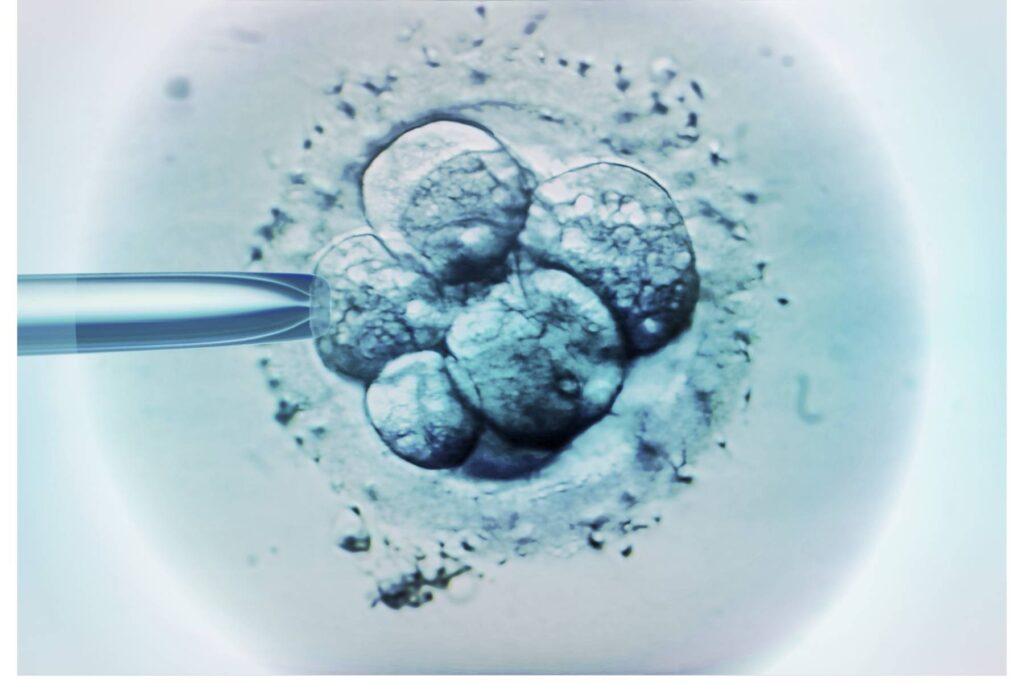
Step 7: Embryo Transfer
If your embryo develops in the lab, the next step is to transfer it into your uterus. This simple procedure is called an “embryo transfer.”
Your fertility nurse will give you instructions on how to prepare.
The embryo transfer is a quick process, like a pap smear. The procedure only takes about five minutes. A scientist gets your embryo ready by placing it in a small tube called a catheter. It’s important that an expert does this to avoid disturbing the embryo.
Your fertility specialist then places the catheter through your cervix and into your uterus.
That’s all there is to it!
You’ll be awake, and there’s no need for anaesthetic. You can get up right away. Feel free to continue with your day; the embryo is secure in your uterus and won’t fall out if you stand up or use the toilet.

Step 8: Pregnancy Test & Follow-up
About two weeks following your embryo transfer, you will undergo a blood test to check your HCG (human chorionic gonadotropin) hormone levels. The presence of HCG in your blood typically suggests a positive pregnancy result. Your nurse will inform you of the specific time for your blood test, as it might differ for certain patients.
Who Needs IVF?
Your fertility specialist may advise you on IVF if you have:
- Blocked or damaged fallopian tubes
- Low sperm count or poor sperm quality
- Endometriosis-related infertility
- Uterine fibroids or polycystic ovarian syndrome (PCOS)
- Advanced maternal age or unexplained infertility
- Recurrent pregnancy loss
- Genetic concerns requiring embryo screening
How do I Prepare for IVF?
IVF can be an overwhelming experience, but we are here to guide you to prepare physically, mentally, and financially.
- Learn About the Process: Once you understand IVF, you will feel less stressed and more prepared for what is next.
- Select the Right Clinic: Choose one with a high success rate, well-experienced doctors, and the most advanced technology.
- Plan Your Finances: Fertility treatments can be quite expensive. Check if your insurance covers them or explore financing options.
Lifestyle Changes to Enhance Chances of Success in IVF
- Eat Healthily: It includes fruits, vegetables, whole grains, and lean proteins in your meals to boost fertility.
- Exercise Regularly: You can choose moderate activities like walking or yoga to improve blood flow and lower stress.
- Manage Stress: Use meditation, deep breathing, or journaling to balance your emotions.
- Avoid Harmful Habits: Quit smoking, reduce alcohol, and avoid recreational drugs as they can lower fertility rates.
How to Stay Emotionally Strong During IVF?
- Talk to Someone: Share your feelings with your partner, close friends, or a support group.
- Seek Counselling: A professional therapist can help manage anxiety and emotional ups and downs.
- Practice Self-Care: Take time for relaxing activities, like reading, listening to music, or taking a warm bath.
What to Expect During the IVF Process?
- First Consultation: Discuss your medical history and undergo fertility tests before beginning treatment.
- Ovarian Stimulation: Take fertility medications to encourage egg production.
- Egg retrieval: The collected eggs are available once matured and are retrieved using a simple process.
- Fertilization and embryo transfer: The eggs fertilized in a lab are left to develop before the best-quality embryo is transferred to the uterus.
- Two-week wait: A pregnancy test confirms success following embryo transfer